
Everything You Need to Know About Mammograms
Learn More
What You Should Know About Birth Control
Learn More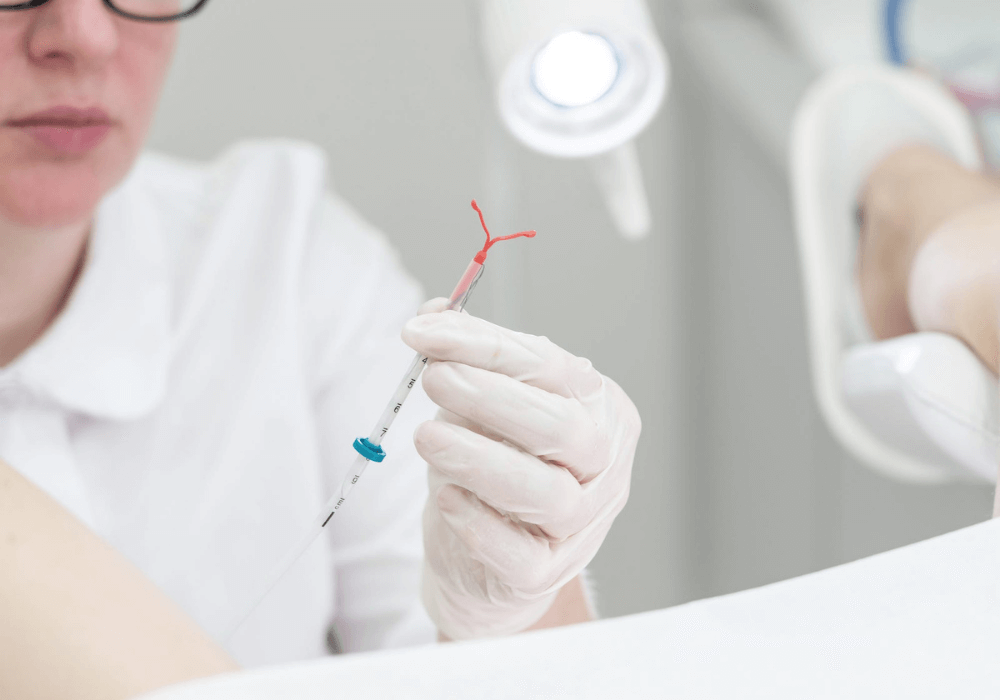
What You Can Expect After IUD Removal
Learn More
Birth Control Can Help With Acne. Here Are Your Best Options
Learn More
Top 5 Women’s Health Myths Debunked by a Gynecologist
Learn More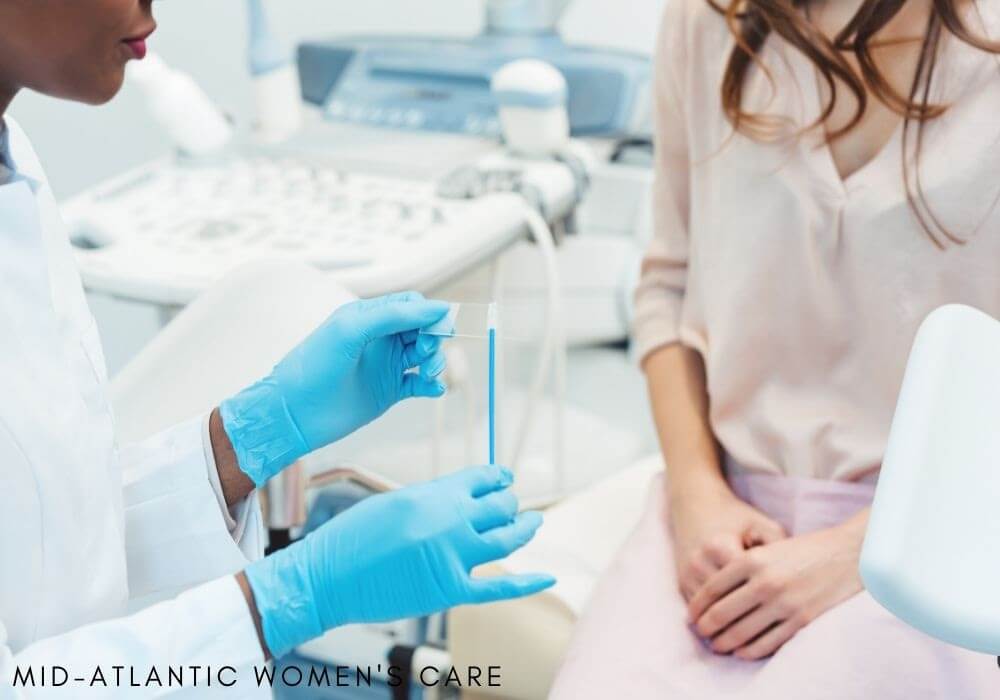
How Often You Should Get Tested for STIs
Learn More
Your Questions About Endometriosis Answered
Learn More
What You Need to Know Before Getting an IUD
Learn More